Test Your Heart Health Knowledge
Cardiovascular disease—including heart attack and stroke—is the leading cause of death worldwide. In the United States alone, one person dies from cardiovascular disease every...
Sedentary Behavior Linked to Higher Risk for Multiple Health Problems
Metabolic syndrome is a cluster of conditions that increase risk of heart disease, stroke, and type 2 diabetes. It is diagnosed by the presence...
Tight Blood Pressure Control is Important at Any Age
High blood pressure is a well-established risk factor for cardiovascular diseases, so treating it is an important strategy for preventing heart attack and stroke....
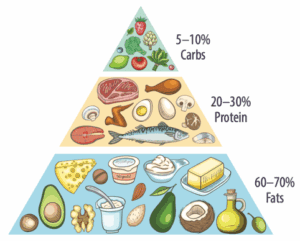
“Keto” Diet for Weight Loss?
If you are following—or considering—a “keto” diet for weight loss, it’s important to understand what research has found out about potential risks and benefits.
What...
The Humble Hamburger
It’s hamburger season! For many people, Memorial Day, Fourth of July, and other warm weather celebrations are not complete without burgers on the grill....
Stress Response is Associated with Heart Attack and Heart Failure Risk
Psychological stress has been linked to both the development and progression of coronary artery disease (CAD). In people who already have CAD (a buildup...
5 Important Fiber Facts
We can’t digest fiber, but it plays a lot of important roles as it passes through the body. Here’s what you need to know:
1....
Preventing Stroke: New Guidelines Released
Every year in the U.S., 600,000 people have a first stroke, and 160,000 die from stroke, making it the fifth leading cause of death...
Any Vigorous Activity May Benefit Women’s Heart Health
Cardiovascular disease (CVD) is the leading cause of death in both women and men globally. In new research, scientists found that brief bouts of...
Modifiable Stroke Risk Factors Should be Addressed
Stroke is a leading preventable cause of disability and death. While one might make a full or near-total recovery from a mild stroke, a...