Eight Essentials for Heart Health
For years we were told to “eat well and exercise” to keep our hearts healthy. While these two lifestyle factors are very important to...
For Brain Health, Protect Your Heart
The same factors that raise the risk for heart disease also impact brain disease, including stroke, Alzheimer’s disease, and other dementias. “Heart disease is...
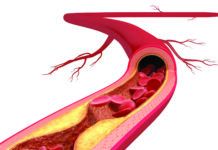
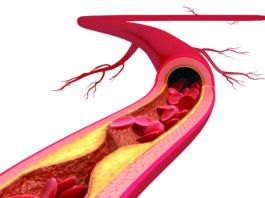
What’s Your ASCVD Risk?
Atherosclerotic cardiovascular disease (ASCVD), commonly referred to as simply cardiovascular disease or heart disease, is a major cause of illness and death in the...
Cholesterol and Genes
Q: It seems like everybody in my family has high cholesterol. I try to eat well and exercise, but my numbers are still high....
Cholesterol, Explained
It’s likely you’ve been told whether you have “high cholesterol.” Perhaps your healthcare provider has discussed your “LDL” or “HDL” levels with you. You...
Newsbites: June 2022
Have High Blood Pressure? Healthy Lifestyle Choices Linked to Lower Risk of Death
A study that followed over 14,000 individuals in China with hypertension (high...
Cardiac Arrest: What You Need to Know
Every year in the U.S., more than 356,000 people of all ages suffer sudden cardiac arrest at home, at work, or while otherwise going...
Newsbites: April 2022
Less Sodium, More Potassium Associated with a Lower Heart Attack and Stroke Risk
A study released at the end of 2021 found that higher intake...
AHA Releases New Dietary Guidance to Improve Cardiovascular Health
The American Heart Association released their 2021 Dietary Guidance to Improve Cardiovascular Health. The new scientific statement emphasizes the importance of dietary patterns over...
Love Your Heart: Reduce Salt Intake
Chances are you consume too much sodium, which can cause high blood pressure. Putting away the saltshaker is never a bad idea, but the...