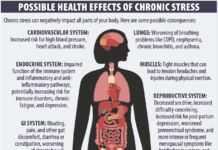
Cancer is the second leading cause of mortality in the United States, accounting for one in four deaths. Lifestyle choices such as use of tobacco products, too much unprotected sun exposure, and excessive alcohol consumption are widely recognized cancer risk factors, but it may be less well known that obesity is considered an important risk factor and poor dietary choices increase cancer risk.
The Role of Diet: A study published recently in the Journal of the National Cancer Institute Cancer Spectrum evaluated the cancer burden associated with various dietary factors. “Our study estimated that more than 80,000 new cancer cases among U.S. adults in 2015 could be attributable to suboptimal diet,” says study author Fang Fang Zhang, MD, PhD, an associate professor at the Friedman School and a cancer epidemiologist. “This accounts for more than five percent of all new cancer cases among U.S. adults in that year.” The number of diet-associated cancer cases was highest among adults aged 65 years and older.
The study found that low consumption of whole grains contributed to the largest number and proportion of diet-associated cancer cases, followed by low consumption of dairy foods. American’s whole grain consumption has improved in the past decade, but it still falls far short of the recommended intake of three servings per day. The current level of dairy consumption among U.S. adults is less than half the recommended three daily servings. “Our estimates suggest that increasing dairy consumption to the recommended level would result in a meaningful reduction in colorectal cancer cases among U.S. adults,” says Zhang. (Some cancer guidelines do not explicitly recommend an increase in dairy consumption because of limited evidence that dairy consumption may increase the risk of prostate cancer.)
Low consumption of vegetables and fruits also contributed to diet-associated cancer cases. Plant foods are good sources of vitamins, minerals, and biologically active compounds that may help protect cells from cancer-promoting damage. “Increasing intake of vitamins, minerals, and phytochemicals should be done with dietary changes, not by taking supplements,” says Joel B. Mason, MD, a professor at the Friedman School and director of the Vitamins and Carcinogenesis Laboratory at the Jean Mayer USDA Human Research Center on Aging. “There is some suggestion that, while low intake of certain micronutrients is harmful, excessively high intake of these same nutrients may be harmful as well. It is practically impossible to reach potentially dangerous excessive amounts of micronutrients through diet.”
- esophagus
- pancreas
- colon and rectum
- endometrium
- kidney
- postmenopausal breast
- gallbladder
- ovarian
- liver
- prostate (advanced)
- stomach
- mouth/larynx/pharynx
High consumption of red and processed meats and sugar-sweetened beverages was associated with higher cancer risk. Intake of red meat (beef, pork, lamb) in the U.S. has been trending downward, but the consumption of processed meats remained unchanged in the past 15 years. According to a 2016 study by Tufts researchers and others, U.S. adults consumed, on average, about one ounce (oz) of processed meats daily. This is more than twice the intake recommended by the American Heart Association (less than half an ounce per day). Intake of sugar-sweetened beverages is strongly associated with obesity, so, given obesity’s clear association with cancer (see below), limiting intake of sweet drinks is an important dietary choice for cancer prevention.
Although it was not measured in this study, the American Institute for Cancer Research (AICR) stresses that there is clear and convincing evidence that alcohol in any form is a potent carcinogen linked to six different cancers, including breast cancer. The AICR advises that those concerned about cancer not drink alcohol, or at least limit intake to one drink for women and two for men per day.
Obesity: “In addition to increase one’s risk of developing certain types of cancer, poor diet contributes to overweight and obesity,” says Zhang. Body fat doesn’t just sit there, it is a metabolically active organ. Fat cells produce estrogen, high levels of which are linked to risk of some cancers. They also produce a variety of proteins that may increase levels of insulin and other hormones, which in turn may spur cancer cell growth. Other substances produced by fat cells can cause chronic inflammation, which is associated with increased cancer risk. Visceral fat—the kind that is typically concentrated in the waist region—is the most metabolically active type of fat tissue. It churns out growth stimulants that encourage cell division—and the more often cells divide, the more opportunity there is for a cancerous mutation to occur.
Along with being more active, avoiding tobacco products, and using sunscreen, the American Institute for Cancer Research recommends the following tips for reducing cancer risk:
- Be a healthy weight. Next to not smoking, maintaining a healthy weight is the most important thing you can do to reduce your risk of cancer. Aim to be at the lower end of the healthy Body Mass Index (BMI) range of 18.5 to 24.9.
- Eat a diet rich in whole grains, vegetables, fruits, and beans. When preparing a meal, fill at least two-thirds of your plate with vegetables, fruits, whole grains, and beans.
- Limit consumption of processed foods. There is strong evidence that consuming processed foods—including “fast food” and refined grain baked goods and snacks—are causes of weight gain, overweight, and obesity, which are linked to 12 cancers.
- Limit consumption of red and processed meat. Eat no more than 12 to 18 ounces (cooked) per week of red meat, such as beef, pork, and lamb. Eat little, if any, processed meat (like ham, bacon, salami, hot dogs, and sausages).
- Limit consumption of sugar-sweetened beverages. There is strong evidence that consuming sugar-sweetened beverages causes weight gain, leading to overweight and obesity. Drink mostly water and unsweetened beverages.
- Limit alcohol consumption. If you do choose to drink alcohol, however, limit your consumption to one drink for women and two for men per day. Do not binge drink.
- Be physically active. Activity may help prevent some cancers, and it helps with weight control to reduce overall cancer risk. Aim for 150 minutes a week of moderate exercise. Any increase over your current activity level helps.
- Do not use supplements for cancer prevention. Aim to meet nutritional needs through diet alone. No dietary supplement has been independently shown to lower cancer risk.
Excessive body weight is estimated to be responsible for seven to eight percent of the cancer burden in the U. S. “There is strong evidence to suggest obesity increases the risk of a number of types of cancers,” says Zhang. “In addition, new studies suggest that obesity-related cancers are rising disproportionately in younger adults. If this trend continues, we expect to see an increase in obesity-associated cancers attributable to suboptimal diet in the next decade.”
Obesity does not impact all cancers, or all people, equally. “While a number of different types of cancers are promoted by excess fat stores, they are not all impacted equally,” says Mason. “The risk for endometrial cancer increases about 350 percent with obesity, while the risk for colon cancer increases 20 in women and 50 percent in men. (For reasons we don’t understand, obesity tends to promote the risk of colorectal cancer more in men than in women. This observation has been seen in a number of different studies, but it’s not clear why it exists.)”
The American Cancer Society recommends avoiding excess weight gain at all ages. For those with overweight or obesity, losing even a small amount of weight has health benefits. In addition to a healthy diet, regular physical activity is strongly recommended. Physical activity not only helps to prevent weight gain and obesity, it also may reduce the risk of several types of cancer, including breast, colon, endometrial, and advanced prostate.

Photography Images © Vadzim Kushniarou |© DNY59 | Getty Images
Inflammation Connection: “We know that organs afflicted by chronic inflammation are at increased risk of cancer,” says Mason. “For example, chronic viral hepatitis (inflammation of the liver) increases liver cancer risk, and the inflammatory bowel disease ulcerative colitis increases risk of colon cancer.” Mason and colleagues recently published a study that found elevated levels of inflammatory markers in the colons of 26 obese individuals but not in 16 of their lean peers. Using blood samples and colonic biopsies, the researchers determined that the concentrations of two major inflammatory proteins rose as body mass index (BMI) rose. “We have known for a couple decades that obesity creates a state of low-grade chronic inflammation in the bloodstream and fat tissue,” says Mason. “This study supports our findings in mice that inflammation also exists within the lining of the colon of individuals with obesity.” While modest in size, this study provides new evidence that obesity promotes cancer through inflammation.
The Bottom Line: Increasing intake of whole grains, dairy, vegetables and fruits—while decreasing intake of processed meats, sugar-sweetened beverages, alcohol, and red meats—is a good idea for those wishing to decrease cancer risk, along with risk of cardiovascular disease and diabetes. These dietary shifts may also help with weight loss in those with overweight or obesity, which is essential to decreasing cancer risk as well as overall health.