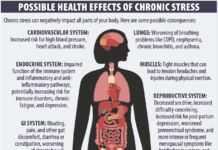
If you sometimes suffer a burning sensation behind your breastbone, you’re far from alone. An estimated 44% of American adults suffer heartburn at least once a month, and about 20% have a serious form called gastroesophageal reflux disease (GERD).
Many sufferers treat their symptoms with over-the-counter or prescription drugs: The generic version of the heartburn medication Prilosec is the sixth most commonly prescribed drug, and acid-suppressor Nexium is second only to Lipitor in total sales dollars. But recent studies have shown that long-term use of medications for heartburn and GERD can block essential nutrients and increase bone-fracture risk.
“Heartburn and GERD are caused by stomach acid refluxing up into the esophagus, thereby causing damage to the surface lining of the esophagus,” explains Robert M. Russell, MD, professor emeritus at Tufts’ Friedman School. Because of the downsides of heartburn medications, he says, you may want to try dietary and lifestyle changes first, or in combination with occasional medication use.
Dreamstime.comDreamstime.com

WHAT IS GERD?
Your diet doesn’t cause GERD, but certain foods can trigger its painful symptoms such as heartburn. Occasional heartburn may be uncomfortable but is nothing to worry about, according to the National Institute of Diabetes and Digestive and Kidney Diseases. If you get heartburn more than two days a week, however, you should tell your doctor.
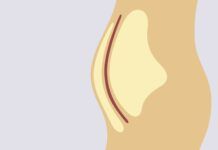
Heartburn – which has nothing to do with your heart – is also known as gastroesophageal reflux (GER), acid indigestion, acid reflux, acid regurgitation and heartburn reflux. By whatever name, it’s caused by a weak lower esophageal sphincter or one that relaxes when it shouldn’t. This sphincter, a ring of muscle, ordinarily acts as a valve between the esophagus and the stomach, opening to let through the food and liquids you swallow. With heartburn, that one-way passage becomes bidirectional. (See illustration.)
Frequent heartburn could be a sign of GERD, in which stomach acids flow up into the esophagus so often that they can cause damage. Other symptoms of GERD include:
– Regurgitation of gastric acid or sour contents into the mouth.
– Difficult and/or painful swallowing.
– Chest pain.
– Chronic cough, caused by acid refluxing up and getting into the lungs. Some GERD sufferers also experience hoarseness in the morning, or a feeling like something stuck in the throat.
– Bad breath.
– Nausea or vomiting.
You may not experience any or most of these symptoms. On the other hand, some people with GERD have these symptoms without the frequent heartburn.
GERD symptoms should not be ignored, as the untreated condition can lead to serious complications. Damage to the esophagus can scar and narrow it, making swallowing difficult, and the inflammation can cause bleeding or ulcers. GERD can also be a precursor to a condition called Barrett’s esophagus, which in turn can lead to esophageal cancer.
To learn more, see: “Vitamin G – Definition Glossary”
GERD MEDICATIONS AND FRACTURES
Reducing the level of stomach acids by medication seems like a natural way to counter heartburn and the risks of GERD, but studies have raised red flags about the consequences of long-term use of such drugs. By blocking stomach acids, these medications can also interfere with the absorption of key nutrients.
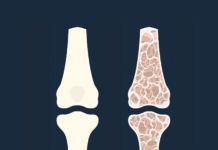
Calcium is one such worry. A study published in JAMA reported that people over the age of 50 who took the most popular type of acid suppressor drugs for a year or more had a significant 44% increase in their risk for breaking a hip. The class of drugs cited in the study—proton pump inhibitors (PPIs) – includes such familiar brands as Nexium, Prevacid and Prilosec.
The study also found a similar but slightly smaller increased risk of hip fracture among users of other acid-suppressing medications known as histamine 2 receptor agonists (H2RA), such as Tagamet and Pepcid. Patients using H2RA drugs for longer than one year had a 23% higher risk for hip fracture.
Researchers said their findings emphasize the importance of lifestyle and dietary modifications as the first option for combating GERD. They strongly cautioned against patients going off or reducing their medications without first discussing with their doctors (particularly if these medications were recommended by their doctors) out of concerns over hip fractures, however. For some, PPIs can be life-saving treatments by preventing peptic ulcers.
If you just take PPIs for a month or so for occasional heartburn and reflux, in any case, there’s little reason to worry. Short-term use was unlikely to have a significant impact on fracture risk, even at high doses of medication. Generally, patients taking PPIs do so for an average of about two months. If your doctor recommends PPI medications, make sure you’re getting enough calcium in your diet and from supplements if necessary.
GERD: POSSIBLE NUTRIENT DEFICIENCIES
Another nutrient of concern is vitamin B12. Between 10% and 30% of adults over age 50 have a condition called atrophic gastritis, which decreases the secretion of hydrochloric acid in the stomach. Taking medications to reduce stomach acid levels has a similar effect. Either way, without enough stomach acids, the body can’t extract adequate vitamin B12 from foods.
Your body needs B12 for proper blood-cell formation, neurological function, DNA synthesis and other tasks. Although B12 is a water-soluble vitamin, when naturally present in foods such as meat, fish, poultry, eggs and dairy products, B12 is bound to proteins in the food. In your stomach, hydrochloric acid and pepsin (an enzyme that breaks down proteins) release the B12 for your body to use.
If you’re taking PPIs or H2RAs for heartburn or GERD, be aware of your body’s B12 demands. Fortunately, the vitamin B12 found in fortified foods, such as breakfast cereals, is different from the natural form. The crystalline synthetic form added to foods or used in supplements is already in a free form that doesn’t require stomach acids for the body to use it.
Other nutrients whose absorption might be reduced by such medications include folate, beta-carotene, vitamin C, magnesium, iron and zinc. Make sure to choose foods rich in the nutrients you may be lacking, including dairy products, green leafy vegetables, whole grains and fortified breakfast cereals. Discuss with your doctor whether you should consider any dietary supplements. In many cases it is not necessary.
Dreamstime.comDreamstime.com

GERD DIET: EATING TO FIGHT GERD
Given the nutritional downsides of long-term use of these medications, it makes sense to try dietary and lifestyle modifications to fight heartburn and GERD. Although foods don’t cause the underlying esophageal sphincter problems, certain foods can trigger your painful symptoms. Some lower the sphincter pressure between the stomach and esophagus, making it easier for stomach acid to reflux up; these can include high-fat foods, alcohol, peppermint, onions, carbonated beverages and chocolate. Other foods, such as citrus and spicy dishes, stimulate the already irritated nerve endings in the lining of the esophagus. Common beverages such as coffee (both caffeinated and decaffeinated), tea, cola, tomato juice and orange juice may also aggravate symptoms.
Other steps you can take to help control your GERD symptoms include:
– Eat more frequent lighter meals and snacks. Large quantities of food are more challenging and take more time to digest.
– Work to lose weight. Cutting calories from unhealthy sources such as starches and added sugars can reduce your risk for heartburn and GERD, which have been linked to being overweight.
– Try chewing gum after meals to stimulate saliva production. Your saliva contains compounds that help neutralize stomach acids and increase peristalsis, the process that moves contents from the stomach to the small intestine. Pick a flavor other than peppermint.
– Follow your meals with a small glass of water. This could help dilute and wash down any refluxing stomach acids.
– Skip carbonated beverages, especially with meals. Carbonation can bloat the abdomen, pressing on your stomach and pushing stomach acids upward.
– Try eating more fiber. One study found that people whose diets were high in fiber were less likely to have heartburn and GERD symptoms, regardless of their body weight.
– Don’t lie down within three hours of eating, when acid production is at its peak. If you’re an early-to-bed person, plan early dinners. You should also avoid bedtime snacks.
– When you do lie down, try keeping stomach acids in their place by raising the head of your bed six to eight inches. Extra pillows under your head probably won’t do the trick; special foam wedges, sold in bedding stores and through medical supply houses, are needed to raise your upper body enough. Or do it yourself by putting blocks of wood under the bedposts at the head end.
– If you smoke, here’s another reason to quit. The chemicals in cigarette smoke may relax the esophageal sphincter and allow reflux of digestive acids.
– Avoid tight-fitting waistbands and clothes that squeeze your middle.
– “Check with your doctor to find out if you are taking any medication that could be promoting heartburn,” says Tufts’ Dr. Russell. “There might be an alternative you could take.”
These small changes in your lifestyle could pay big dividends in your quality of life, reducing discomfort and possibly long-term risks to your health.
To learn more, see: “Eat Right to Fight Heartburn and Reflux”
For more information on heartburn and GERD:
–International Foundation for Functional Gastrointestinal Disorders,
–National Institutes of Health, (800) 860-8747