Low-Carb Mediterranean Diet Works as Well as Ketogenic Diet for Diabetes Control
In a controlled trial comparing a well-formulated ketogenic diet with a low-carbohydrate Mediterranean-style dietary pattern for 12 weeks, both diets helped people with type 2 diabetes or prediabetes control blood sugar levels and lose weight.
Both diets were low in refined grains and added sugars and high in nonstarchy vegetables. The ketogenic diet also avoided fruits, legumes, and whole grains, while the Mediterranean diet included these foods. Prepared meals were provided for the first four weeks of each diet, with dietary recommendations for the next eight weeks.
Both diets improved long-term blood sugar control (measured by hemoglobin A1c), fasting insulin and glucose, HDL (good) cholesterol, and the liver enzyme ALT. Both diets also led to similar weight loss. Triglyceride levels decreased on both diets (which is desirable) but went down more on the ketogenic diet; while LDL (bad) cholesterol decreased on the Mediterranean diet but increased on the keto diet.
Overall, the investigators concluded that both diets were effective for glucose control, but the Mediterranean-style diet included more health-promoting foods, variety, and higher amounts of fiber, phosphorus, thiamin, and vitamins B6, C, D, and E. The Mediterranean-style dietary pattern in this study was also easier for participants to follow long term. These new results suggest that a low-carb Mediterranean-style dietary pattern may be helpful for people with type 2 diabetes.
Using a Saltshaker at Meals Associated with Shorter Lifespan
Researchers analyzed the salt-using habits of 501,379 people in the United

For a longer, healthier life, leave the saltshaker off the table.
Kingdom. Those who reported more frequently adding salt to foods at the table (not including salt used in cooking) had higher concentrations of sodium in their urine (a finding that supports the self-reported intake). In the nine years of follow-up, there were 18,474 premature deaths (younger than age 75). The more frequently people reported adding salt to foods, the higher their risk of premature death. This association was most pronounced in people who also reported low intake of fruits and vegetables. (Low fruit and vegetable intake would be associated with low intake of potassium, a mineral that helps mitigate the harmful effects of sodium). Whether the excess sodium came from table salt or other processed foods more frequently consumed by these individuals could not be determined.
It is well known that high intake of salt (sodium) raises blood pressure in most individuals. High blood pressure increases risk for stroke and heart attack. Sodium intake should be limited to 2,300 milligrams a day (or less if you have high blood pressure).
Maintaining a Healthy Lifestyle May Offset Genetic Risk of Prostate Cancer
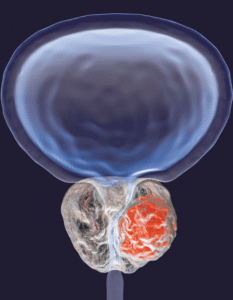
Even if you are at genetic risk, lifestyle choices may reduce risk of dying of prostate cancer.
Prostate cancer has a strong genetic component. A prospective study that followed over 12,000 men for 27 years found that a healthy lifestyle was associated with lower prostate cancer risk, even in men at high genetic risk. A healthy lifestyle was defined as maintaining a weight below the obesity cutoff (BMI <30), regularly engaging in vigorous physical activity like jogging or playing singles tennis, not smoking, limiting processed meat intake, regularly eating fatty fish (like salmon), and eating tomato products (which have been associated with lower risk of prostate cancer).
About one in eight men will be diagnosed with prostate cancer in their lifetime, and one in 41 men die of this slow growing disease. In this study, men with the highest genetic risk for prostate cancer were over four times more likely to die of the disease than those with the lowest genetic risk. A healthy lifestyle made a significant difference. In men with the highest genetic risk, those who had a healthy lifestyle had a lifetime risk of dying from prostate cancer of 1.6 percent, compared to 5.3 percent for those high-risk men with an unhealthy lifestyle. Among men with a high genetic risk, those who engaged in the most healthy lifestyle activities had 45 percent lower odds of dying from prostate cancer than those who engaged in the least.
Whether or not you have a family history of prostate cancer, a healthy lifestyle is a great way to lower your risk for this disease and many others.