We all know that diet and physical activity are essential to good health, but many are unaware that getting adequate sleep is equally important, if not more so. Sleep affects everything from energy and appetite to performance, mood, attention, memory, and decision making. It is the time when the brain forms and maintains the pathways that let us learn and create new memories. Recent research suggests that the body uses sleep time to remove toxins and metabolic “trash” from the brain (possibly including the plaques that contribute to Alzheimer’s disease). Habitual short sleep duration is associated with greater risk of obesity, high blood pressure, diabetes, depression, and cardiovascular disease. Unfortunately, about one third of U.S. adults get less than the recommended seven hours of sleep a night.
“While we don’t understand everything about sleep, we know it is essential for life,” says Jos Ordovs, PhD, a professor at the Friedman School and director of the Nutrition and Genomics Laboratory at the Jean Mayer USDA Human Nutrition Research Center on Aging. “We can survive extended periods of time without eating but we cannot go for very long without sleeping.”
How Sleep Works: When we’ve been awake for a long time, we begin to get sleepy; our bodies then try to maintain sleep long enough that we wake up restored and rested. This process is controlled by an internal biological mechanism called sleep/wake homeostasis. Medical conditions, medications (including some for high blood pressure and asthma), stress, sleep environment, and even what we eat and drink can influence sleep-wake needs. Exposure to light is especially critical. Our circadian rhythms respond to light and darkness, releasing hormones to help us feel awake (like cortisol and adrenaline) or promote sleep (like melatonin and GABA). This internal ‘biological clock’ works with sleep/wake homeostasis to regulate the timing of periods of sleepiness and wakefulness throughout the day. If you tend to get sleepy in the afternoon no matter how much sleep you’ve gotten (or feel great early in the morning despite not getting much sleep), that’s your circadian rhythms at work. Travelling between time zones disrupts circadian rhythms, and so does keeping long and irregular hours.
Not all time spent sleeping is the same. For the first five or 10 minutes after we doze off we are in stage one of sleep—the transition phase; people often insist they were not asleep when awakened during this stage. Stage two, which makes up about 50 percent of sleep time, is also light; the heart rate slows and body temperature drops, preparing the body for deep sleep. Stage three—deep sleep—is where much of the important work is done. It is divided into periods of rapid eye movement (REM) sleep and non-REM sleep. The brain is very active during REM sleep, and this is when dreams occur. Scientists aren’t sure why we dream, but they suspect it has something to do with helping us processes emotions. During non-REM sleep, the body repairs and regrows tissues, builds bone and muscle, and strengthens the immune system. Throughout our time asleep, we cycle through periods of light stage, REM, and non-REM sleep.
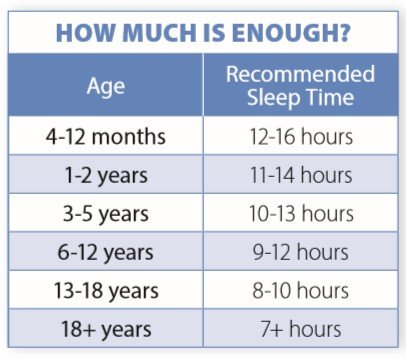
“Sleep needs vary with age,” says Ordovs. “We know that babies, young children, and adolescents need more sleep than older adults.” (See How Much is Enough? below)
While some sleep disorders have environmental or behavioral triggers, several genes have been identified that influence our circadian rhythms, the timing of sleep, and susceptibility to sleep disorders. It is important to seek diagnosis and treatment if you have trouble with sleep.

Image © Dirtydog_Creative | Getty Images Image © SiberianArt | Getty Images
Sleep, Hunger, and Weight: Getting an adequate amount of quality sleep is an often-overlooked tool for helping maintain a healthy weight. “Reduced sleep has been shown to alter the hormones involved in hunger and satiety, along with subjective hunger and preferences for ‘comfort foods’ including highly processed junk and snack foods,” says Dariush Mozaffarian, MD, DrPH, dean of the Friedman School and editor-in-chief of Tufts Health & Nutrition Letter. In a prospective cohort study published in 2011 in the New England Journal of Medicine, Mozaffarian and colleagues looked at weight gain over 20 years in more than 120,000 men and women. “Our study found that, after adjusting for other factors, people who slept less than six hours per night had significantly greater weight gain than people sleeping six to eight hours per night.”

Image © DrAfter123 | Getty ImagesImage © LIgorko | Getty Images
A 2015 study by Ordovs and colleagues found that longer habitual sleep was associated with lower body mass index (BMI). Several studies point to late-night snacking and less-healthy food choices as part of the problem. Research suggests that hormonal changes related to inadequate sleep time could increase the desire to munch: while not all studies agree, some early research found that levels of leptin (a hormone that helps us feel full) decreased with sleep deprivation, and levels of ghrelin (known as the “hunger hormone”) increased. Whatever the reason, lab studies that restricted participants to less than six hours of sleep found an increased intake of 300 to 550 calories a day, mostly from late-night snacking. This could translate to weight gain of around a pound a week. On the positive side, the study by Ordovs and colleagues mentioned above suggests that longer habitual sleep may help overcome some genetic variants that predispose people to obesity.
Sleep and Health: In addition to weight gain, short sleep duration has been associated with numerous health problems. Meta-analyses indicate a 30 percent increased risk of diabetes in people who sleep less than five to six hours a day, and in those who sleep more than eight hours a day. Several studies and meta-analyses have reported associations between short sleep duration and high blood pressure (but no such association has been reported with long sleep duration). Analysis of medical records of over 31,000 adults found that short sleep duration was independently associated with atrial fibrillation, an irregular heartbeat that increases risk of heart failure, kidney problems, stroke, coronary heart disease, and death.
A small recent study found that deep sleep helps relieve anxiety, and a sleepless night can raise subjective anxiety by up to 30 percent. Brain scans on 18 sleep-deprived young adults revealed deactivation of a brain area linked to calming anxiety and stress, and excessive brain activity in regions associated with processing emotions. After watching emotionally unsettling videos, participants reported much lower anxiety levels after a full night’s sleep than after a sleepless night, especially if they had gotten more deep, non-REM sleep.
A 2019 study by Ordovs and colleagues found that lower sleep times and fragmented sleep are independently associated with higher risk of plaque build-up in the arteries (atherosclerosis). The researchers performed sleep studies on nearly 4,000 participants. They also took three-dimensional ultrasounds and CT scans to look for build-up of plaque in the carotid and femoral arteries as well as calcification in the arteries that supply oxygen to the heart muscle. Lower sleep time and fragmented sleep were both associated with plaque build-up in all these areas. “Our research shows that sleep disruption, whether in quantity or quality, has long term, insidious, and dangerous consequences,” says Ordovs. “It promotes the silent buildup of plaques within our arteries, raising the risk of cardiovascular disease, the leading killer in our society.” Moreover, this happens above and beyond the relation of poor sleep with other cardiovascular risk factors such as obesity, diabetes, and hypertension.
“Sleep disruption has some evident short-term consequences,” says Ordovs. “We feel tired, moody, stressed and, of course, sleepy. If we don’t have enough quality or quantity of sleep, which unfortunately is common in our society, our quality of life in the short and long term suffers. In addition, it affects other behavioral factors involved in chronic diseases such as the quality of our diet and our physical activity. Therefore, sleep must be considered as the third pillar of health in combination with nutrition and physical activity.”
SLEEP TROUBLES: Inadequate sleep can come from trouble with either quantity, quality, or both
Insomnia, which can include difficulty falling asleep, difficulty staying asleep throughout the night, or waking up too early in the morning, affects as many as 30 to 35 percent of adults in the U.S., according to the American Association of Sleep Medicine. It is more common in women, people under stress, and people with certain medical and mental health problems (including depression), as well as older adults. According to some sources, chronic insomnia affects 57 percent of older adults in the U.S. Studies show that insomnia negatively affects work performance, impairs decision-making, and can damage relationships. If it takes you 30 minutes or more to fall asleep, or if you’re awake for 30 minutes during the night, at least three times a week for three months, you have chronic insomnia and should seek treatment. The recommended first-line treatment for insomnia is cognitive behavioral therapy, a short-term, goal-oriented psychotherapy.
Sleep Apnea is a common and serious sleep disorder in which people temporarily stop breathing for short periods of time while they are sleeping. The muscles of the upper airway relax during sleep, allowing the tissue at the back of the throat to collapse and block the passage of air to the lungs. People with this condition may snore loudly or make choking or gasping noises, and the oxygen-deprived brain may wake them multiple times throughout the night to restart breathing; they are often unaware they are not sleeping soundly but may wake up feeling unrefreshed and suffer with fatigue throughout the day. Sleep apnea is associated with serious negative long-term consequences, including high blood pressure, heart disease, stroke, diabetes, and depression. Risk for sleep apnea goes up with BMI. Getting diagnosed with an in-lab sleep study or at-home sleep apnea test is critical. This condition is managed using continuous positive airway pressure (CPAP) therapy, an oral appliance, or surgery.
Circadian Rhythm Disorders occur when people’s internal sleep-wake schedule does not align with darkness and light. This misalignment can be caused by jet lag, shift work, damage to the brain, or frequently going to bed and getting up at different times. Delayed sleep phase disorder, seen most often in adolescents and young adults, is characterized by the need to stay up very late and sleep late. Advanced sleep phase disorder, more common among older adults, is characterized by falling asleep and awakening early. These conditions can be diagnosed by a doctor’s evaluation and are usually treated with behavior change and controlling light exposure, although a doctor may prescribe sleep aids and/or drugs to stimulate the brain.
Restless Legs Syndrome causes an overwhelming urge to move one’s legs which interferes with falling asleep. This neurological sleep disorder should not be ignored and can be managed through medication and lifestyle changes.
Parasomnias include sleepwalking, sleep talking, and sleep eating disorder; sleep terrors, nightmares, and sleep hallucinations; sleep paralysis (being briefly unable to move while falling asleep or waking up); confusion arousals (in which people are very confused and behave strangely upon awakening); and the potentially dangerous REM sleep behavior disorder, in which people act out vivid dreams as they sleep. These conditions may interrupt sleep. They can be treated using medication and/or behavioral therapy and lifestyle changes.
Take Charge!
Follow these tips to establish healthy sleep habits:
-Keep a consistent sleep schedule. Get up at the same time every day, even on weekends or during vacations.
-Set a bedtime that is early enough for you to get at least 7 hours of sleep.
-If you don’t fall asleep after 20 minutes, get out of bed.
-Don’t nap too long or too late in the day.
-Establish a relaxing bedtime routine.
-Use your bed only for sleep and sex.
-Make your bedroom quiet and relaxing. Keep the room at a comfortable, cool temperature.
-Limit exposure to bright light in the evenings, including screens. Bright light at night can confuse the brain and prevent the ramping up of melatonin.
-Turn off electronic devices at least 30 minutes before bedtime.
-Don’t eat a large meal before bedtime. If you are hungry at night, eat a light, healthy snack.
-Exercise regularly and maintain a healthy diet.
-Avoid consuming caffeine in the late afternoon or evening.
-Don’t consume much alcohol at bedtime. While alcohol can make you sleepy, it is known to interfere with quality of sleep. Allow enough time for your blood alcohol level to drop before bed.
-Reduce your fluid intake before bedtime.
-Don’t check the clock. If the alarm has not gone off…go back to sleep!

More study is needed on the efficacy of supplements marketed to help improve sleep quantity or quality. There is very little evidence supporting use of over-the-counter supplements and some have serious potential side effects. Note that herbal supplements are not regulated by the FDA and do not need to prove they do what they claim to do. Tell your doctor if you take any supplements. Here is a brief word on several common sleep remedies:
Ashwagandha: Some research suggests this root extract may help reduce cortisol levels, stress, and anxiety, which could help some people with sleep. Pregnant and nursing women and individuals with autoimmune or thyroid disease should not take ashwagandha.
Chamomile: This herb is considered safe and may help with relaxation, but more research is needed to prove its effectiveness for insomnia and other sleep disorders. Do not take if you are allergic to ragweed or chrysanthemums, daisies, or sunflowers.
GABA: While low levels of this neurotransmitter are associated with insomnia and disrupted sleep, it cannot cross the blood-brain barrier, so supplements are useless.
Kava-kava: While this plant extract has been shown to have promising anti-anxiety effects and potential value for the treatment of sleep disorders, serious side effects have been reported, including liver failure that in some cases resulted in death.
Lavender: Several studies suggest that aromatherapy with this flower may improve quality of sleep, but oral supplements are less studied and can cause gastrointestinal side effects.
Magnesium: According to some sources, this mineral may have a relaxing effect, but dietary intake from foods like nuts, seeds, legumes, and avocados should provide enough.
Melatonin: This hormone signals your brain that it’s time to sleep. Taking it as a supplement may slightly improve sleep onset and sleep duration, but product quality and efficacy may vary and long-term safety has not been established.
Valerian: This root seems to be relatively safe and may be of some benefit with mild sleep problems, but study results have been mixed—with more negative results than positive. Valerian can interfere with some medications.


























You do not discuss the affects of need to urinate in the middle of the night and its affect
on the interruption of sleep two or three times per night, even if returning to sleep is quick.
This is my big problem. I would appreciate some comments. 😉
A study done in mice suggests that higher salt intakes result in poorer sleep quality, a factor that could result in more nighttime awakenings. See https://www.physiology.org/detail/news/2021/10/04/high-salt-diet-may-disrupt-body-clock?SSO=Y
Additionally, restricting fluid intake (including especially alcohol) for several hours prior to bedtime should reduce nighttime awakenings to urinate.
Finally, if you have any leg edema (even if relatively minor), wearing compression hose while awake during the day would reduce the accumulation of fluid in the lower extremities, fluid that (once supine) would otherwise migrate to the circulation and, eventually, to the kidneys, resulting in increased urine production.
I highly value your daily newsletter.
Thank you…………
A new-to-me ND has recommended Phosphatidyl Serine to improve sleep. As an active self-advocate for my own health (and a trained researcher) I am looking for any studies that will validate this recommendation.
So what about Arnold Farbers question—-how does urination sensations and getting up to urinate 4 times a night….affect your sleep and what can you do about it…when your urologist tells you I think you have a sleep problem…..REALLY?
Great article. Thank you. Leo
If a person falls asleep on the couch for 2 hours and then goes to bed and sleeps 5 hours is that considered a proper 7 hour sleep or is interrupted sleep not as good??