Our bones support us, literally, in everything we do. They protect our vital organs, store important minerals the body relies upon, and keep us moving. From childhood through early adulthood, our bones are busy taking up nutrients that help them grow, strengthen, and build density. By age 30, bone density has peaked, and it begins to decrease as we age. Bone loss can lead to osteoporosis, the thinning of bone that makes us more susceptible to fractures and potential disability. Fortunately, there’s a lot we can do to help maintain strong, healthy bones.

Image © JulNichols | Getty Images
Staying Strong: The key to building and maintaining bone is using our muscles. “When a muscle works against a force, the bone it is attached to responds,” says Roger Fielding, PhD, a professor of nutrition at the Friedman School. “Cells inside the bone send signals to stimulate bone growth.” Regularly engaging in weight-bearing activities (including walking, running, cycling, and hiking) and strengthening exercises (such as weightlifting, bodyweight exercises like squats and planks, and high intensity training) provide the positive stress bones need. Regular physical activity will also increase muscle strength and coordination. “If older people lose bone and muscle, they get to a critical point where a fall can lead to fracture due to low bone density,” says Fielding. Even a small amount of regular physical activity is better than none at all. While both weight-bearing and strengthening exercises are recommended, Fielding suggests people do what they enjoy. “The key is to be active on a regular basis,” says Fielding. “We are more likely to keep up with an activity if we actually like doing it.”
Eating Well: A healthy diet promotes strong, healthy bones throughout every stage of life. Some foods and nutrients are particularly associated with bone health:
Fruits and vegetables: Fruits and vegetables can help with bone maintenance. A study in 2017 in the journal PLoS One found that fruit and vegetable intake was associated with higher bone mineral density and lower incidence of osteoporosis in middle aged and older adults. Another study published in a 2019 issue of the same journal found an additional serving of fruits and vegetables a day was associated with lower fracture risk. “Whether these associations are a result of the higher intake of fruits and vegetables or the lower intake of other foods that were crowded out can’t be determined,” says Alice H. Lichtenstein, DSc, a professor at the Friedman School and executive editor of Tufts Health & Nutrition Letter. One reason fruits and vegetables may contribute to bone health is their role in maintaining the body’s acid-base balance. Acids increase as kidney function declines (a natural occurrence with aging) and also because of common food preferences: diets high in proteins and grains are acid producing. When acids in the body increase, alkaline compounds are released from bones to neutralize the acid. This weakens the bones. Fruits and vegetables are metabolized to alkaline (basic) products, so eating more of these foods helps maintain acid-base balance. “American diets are out of balance as a rule,” says Bess Dawson-Hughes, MD, director of the Bone Metabolism Laboratory at the Human Nutrition Research Center on Aging. “Grain intake is double the recommended amount, and fruits and vegetables are half the recommended amount.” This imbalance leads to excess acids in the body. Dawson-Hughes suggests eating five to ten servings of fruits and vegetables a day.
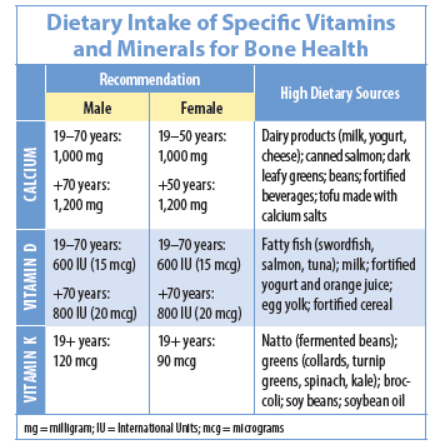
Calcium: Dietary calcium is critical for building bone mass when we’re young and helping preserve it as we age. In addition, it hastens recovery from fracture. Ninety-nine percent of calcium in the body is stored in bones. Calcium is essential to many functions in the body. If a person doesn’t take in the amount of calcium the body needs, the bones will release calcium to make up the difference—fixing the imbalance but weakening the bone.

Images © Iryna Imago | Getty Images
Vitamin D: Vitamin D (D2 and D3) is as important to bone health as calcium because it’s necessary for calcium absorption. Vitamin D is made in the skin when it’s exposed to sunlight. A few foods, including some fatty fish, egg yolk, and liver, contain vitamin D naturally, and it is added to a number of foods, including milk and some dairy foods, cereals, and juices (check the Nutrition Facts label).
Vitamin K: Vitamin K may also be important in the regulation of bone formation. Low blood levels of vitamin K have been associated with low bone density. A review of studies published in 2019 in the Journal of Osteoporosis concluded that most studies find low serum K1 levels and low dietary intake of both K1 and K2 are associated with a higher risk of fracture and lower bone mineral density. One of the studies cited, a 2017 meta-analysis involving more than 80,000 participants, found that men and women with the highest intake of vitamin K had a 22 percent lower risk of fracture.
Protein: Adequate protein intake is important for bone health, but too much protein may actually be bad for bones. Protein helps preserve muscle mass, and, as stated earlier, using muscles helps build bone. Weak muscles increase risk of falls, and insufficient protein has been associated with greater risk of severe hip fracture in older adults (although not all studies agree). Since the breakdown of protein during digestion releases acids into the bloodstream and the body neutralizes these acids by drawing calcium from the bones, too much protein may weaken bone. “Very high intakes of protein are not recommended, particularly for bone health,” says Lichtenstein. “Aim for moderate intakes.” More research is needed to determine what level of protein intake provides the best protection against osteoporosis.
Supplements: “Food is generally the best way to get the nutrients we need,” says Dawson-Hughes. Calcium and vitamin D supplement use is controversial. There are many conflicting reports on the benefits and harms of their use alone or combined for the prevention of fractures in adults. A recent meta-analysis of 11 observational studies published in JAMA Network Open, which included over 39,000 participants, concluded that vitamin D supplementation alone did not reduce risk of fracture, but a combined supplementation of calcium and vitamin D reduced risk of all types of fracture by six percent and hip fracture by 16 percent.
If a person is unable to eat dairy products or calcium-fortified foods, which are the highest source of calcium per serving, then a supplement may be needed to bring them up to the recommended 1,000 to 1,200 milligrams (mg) a day. Likewise, “people at high risk for low vitamin D—such as those who avoid sun exposure, have very dark skin, or are obese—may need more vitamin D,” says Dawson-Hughes.
When it comes to supplements, it is important to avoid the mindset that if a little is good, more must be better. “For vitamin D, neither blood levels that are too low nor those that are too high are good,” says Dawson-Hughes. Calcium intake over 2,000 mg a day has been associated with increased risk of prostate cancer; vitamin K supplements are not generally recommended; and vitamin D and calcium supplements should not be taken without a doctor’s recommendation.
Try these tips to maintain healthy bones:
- Be Active! Daily weight-bearing activities, like walking or hiking, help retain bone mass and encourage bone growth. Strengthening exercises build muscle to help strengthen bone and minimize the risk of falls.
- Aim for 1,000 to 1,200 mg of calcium a day from foods like dairy products, fortified beverages, leafy greens, canned salmon, and tofu set with calcium.
- Take vitamin D and calcium supplements only if a doctor recommends it, and avoid high doses.
- Eat five to 10 servings of fruits and vegetables a day. This may help your body maintain acid-base balance, minimizing bone breakdown.
- Strive for one or more servings of vitamin K rich green leafy vegetables each day to minimize the risk of fractures. Talk to your doctor if you are on anticoagulant medications.
In 2018, the U.S. Preventive Services Task Force on fall and fracture prevention concluded that many older adults should avoid taking vitamin D and calcium supplements to prevent falls and fractures and focus on being more physically active instead. So, aim for a healthy dietary pattern and regular activity to help build and maintain strong bones.
























