Image © Vladislav Lukyanov | Dreamstimecom

The American Heart Association and the American College of Cardiology have released an update to guidelines that redefines high blood pressure (hypertension) and makes recommendations on how doctors should treat it. The guidelines lower the threshold at which a person would be diagnosed with hypertension. Under the new standard, it’s estimated that 46% of American adults can now be diagnosed, or about 100 million people. The guidelines set a lower bar for what will be considered hypertension. Though voluntary, the guidelines are likely to influence how some doctors advise and treat their patients.
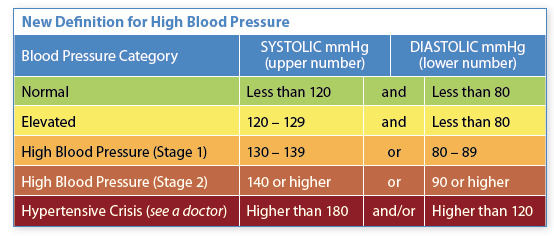
The ideal, healthy blood pressure has not changed: less than 120/80 millimeters of mercury (mmHg). The upper number (systolic pressure) measures the pressure on the artery walls when the heart contracts. The lower number (diastolic pressure) is the pressure on the arteries when the heart relaxes. Staying below 120/80 is associated with reduced risk of cardiovascular disease (heart attack, heart failure, stroke) and kidney failure. Starting at 120/80, the risks rise steadily.
The previous recommendation for defining hypertension was 140/90 or higher. Now, a pressure of 130/80 or higher is considered hypertension, whereas earlier this was known as “pre-hypertension.” The latest research has shown that treating people to get blood pressure below 130/80 is both beneficial and safe—even for those 65 and older, who are more at risk of side effects from blood pressure medications.
Although medication remains an important tool in the treatment of hypertension, the guidelines strongly emphasize the importance of a healthy eating pattern, physical activity and other positive steps for everyone.
“It’s been known for a long time that high blood pressure is essentially a lifestyle disease,” says Dariush Mozaffarian, MD, DrPH, dean of Tufts’ Friedman School and editor-in-chief of Tufts Health & Nutrition Letter. “The new guidelines emphasize that adopting a healthy eating pattern and other lifestyle changes is the front-line defense against hypertension.”
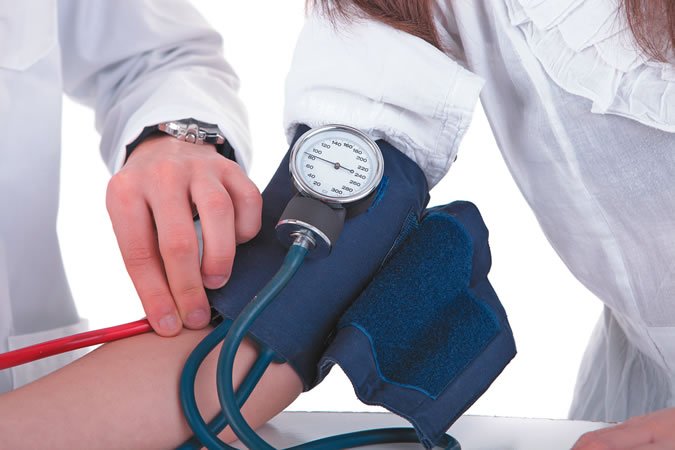
Risks and Benefits: The guidelines came after a review of the latest scientific literature. Safety was a key question. Doctors were concerned that more aggressive” treatment to drive pressures below 130/80 could cause too many side effects. For example, sudden dips in blood pressure caused by medication can lead to fainting spells or falls. Safety is an important consideration for older people. Under the new guidelines, about 80% of women and men 65 and older could be diagnosed with hypertension.
Part of the answer to the question about side effects came from the Systolic Blood Pressure Intervention Trial (SPRINT). The study involved more than 9,300 people 50 and older at high risk of cardiovascular disease. (About 28% of the participants in SPRINT were over age 75.) The participants were randomly assigned to have their high blood pressure treated to get it below one of two target systolic (upper number) blood pressures: either 140 or 120 mmHg.
Participants in the group with a target below 120, compared with those with a target below 140, were less likely to develop heart failure, a condition in which the heart can’t pump enough blood to meet the body’s needs. They were also less likely to die from cardiovascular problems or from any other cause.
The reduced risks did come with more side effects. Participants treated to 120 experienced fainting more often, but there was no difference in the number of falls leading to injury.
What the guidelines advise depends on both a person’s blood pressure and their overall cardiovascular risk. Someone with mildly elevated pressures (120-129 mmHg) would be counseled on lifestyle change. At 130/80 and above, people at relatively low risk of cardiovascular problems would also be advised to first try lifestyle change. However, those found to be at higher risk of cardiovascular problems could be treated sooner and more aggressively.
Lifestyle Treatment: In all cases, lifestyle improvement addresses the underlying causes of high blood pressure. The major factors linked to lower cardiovascular risk are excess body weight, unhealthy eating patterns (particularly excess sodium intake), physical inactivity and alcohol consumption.
Only about half of people treated for high blood pressure under the previous guidelines (below 140/90) are able to reach their targets. The new guidelines raise the bar higher for treatment, but also catch hypertension earlier. Lifestyle changes work, and many people are motivated to change, says Hanna Ahmed, MD, MPH, a cardiologist at Tufts Medical Center.
“I talk to them about the changes that they can make on their own, such as improving their diet, increasing physical activity, losing weight and stopping smoking. Lifestyle changes work to decrease the blood pressure at any level, but medications may be necessary for those who are not able to get to target blood pressure goals with lifestyle changes alone, or for those with baseline higher blood pressure readings.”

Here are actions you can take to address elevated blood pressure, alone or in combination with medication, as your doctor advises:
- Body Weight. Large epidemiological studies have found a direct relationship between above-normal body weight and risk for hypertension. A Body Mass Index (BMI) below 25 is ideal.
- Physical Activity. Increased physical activity lowers the risk for hypertension. The recommended target for Americans is 150 minutes of moderate exercise (such as walking, light jogging, housework or gardening) per week or 75 minutes of strenuous exercise (gym workouts, for example, or vigorous lap swimming).
- Diet. What you eat, particularly sodium, affects your risk for high blood pressure. The National Institutes of Health has developed a specific diet for lowering high blood pressure: Dietary Approaches to Stop Hypertension (DASH). It’s high in fruits, vegetables and low-fat dairy foods and high in potassium. In a clinical trial of the DASH diet, it lowered systolic blood pressure by about 10 mmHg and diastolic pressure by about 5 mmHg. That’s comparable to the minimum effect of taking a blood pressure medication. In studies, reduced-sodium versions of the DASH diet work even better.
- Potassium. An adequate amount of potassium in your diet is recommended to prevent and treat hypertension. The new blood pressure guidelines advise adults to aim for 3,500 to 5,000 mg of potassium per day.
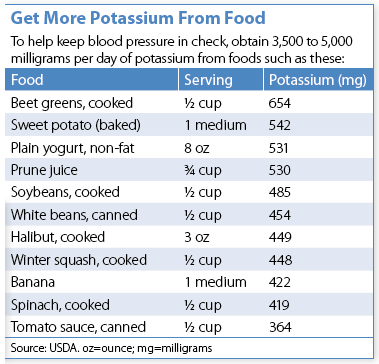
“Right now it appears that it’s not only sodium; it’s also potassium,” says Alice H. Lichtenstein, DSc, director of Tufts’ HNRCA Cardiovascular Nutrition Laboratory. “However, much less is known about potassium. There’s no evidence to suggest that if you take a potassium supplement you’re going to lower your blood pressure, but it does appear that if you eat more foods that are lower in sodium and higher in potassium, you have improve your blood pressure.”
- Alcohol. The new blood pressure guidelines note that alcohol consumption may account for a significant number of cases of hypertension in the US. Guidelines suggest limiting daily intake to 1 standard drink if you are a woman and 2 drinks if you are a man. A standard drink is 12 ounces of beer, 5 ounces of wine, or 1.5 ounces of 80-proof spirits.

Try these 4 simple steps to reduce your sodium intake:
-Avoid food products high in sodium by reading Nutrition Facts labels. (See The Salty Six below.)
-Choose canned foods marked reduced sodium, low sodium, or no sodium.
-Use herbs and spices to add flavor to foods, which can reduce the amount of salt you add.
-When cooking from recipes, cut the specified amount of salt by half.
The Salty Six: The American Heart Association has identified the following foods as the salty six that contribute a significant amount of sodium to the American diet. Check nutrition information, reduce portions and look for reduced-sodium options
-Breads and rolls
-Canned soups and broth
-Cold cuts and cured meats
-Pizza
-Poultry with added sodium, such as pre-seasoned fillets and chicken nuggets
-Sandwiches and burgers from fast-food restaurants

























I am 84plus. I am having BP 74-145’.some times in the evening BP rises to 84-170 I feel odd. I am taking TelzeAM in the morning .After going through the above.I could understand that my diet needs improvement.Thanks.