Atherosclerotic cardiovascular disease (ASCVD), commonly referred to as simply cardiovascular disease or heart disease, is a major cause of illness and death in the United States. Knowing your risk can help you and your healthcare provider determine the best ways to lower that risk and prevent ASCVD from occurring.
What is ASCVD? ASCVD is characterized by atherosclerosis, the buildup of plaques in 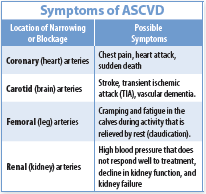 artery walls. These plaques can partially or completely block the flow of blood in the arteries. They can also block blood flow by triggering the formation of blood clots. The consequences of ASCVD depend on where and how quickly the blockage or narrowing occurs (See Symptoms of ASCVD table for more information).
artery walls. These plaques can partially or completely block the flow of blood in the arteries. They can also block blood flow by triggering the formation of blood clots. The consequences of ASCVD depend on where and how quickly the blockage or narrowing occurs (See Symptoms of ASCVD table for more information).
Risk Factors. There are many risk factors you can control to change your risk of ASCVD. Quitting smoking is best, but reducing the numbers of cigarettes smoked per day and even periods of temporary quitting lower risk. Other major risk factors include high blood pressure, abnormal blood cholesterol levels (for example, high levels of LDL cholesterol and triglycerides and low levels of HLD cholesterol), diabetes, prediabetes, and lifestyle behaviors including an unhealthy dietary pattern, being inactive, and having excess body fat. “Each of these risk factors are independent,” says Dariush Mozaffarian, MD, DrPH, dean for policy at the Friedman School and editor-in-chief of this newsletter. “In other words, all contribute to risk, regardless of the levels of the others.”
Your age is also a top determinant. “Risk goes up steeply in both men and women with
Other risk factors for which evidence is not yet fully established include mental stress, poor sleep, and depression. Prior conditions like diabetes during pregnancy (gestational diabetes)or inflammatory conditions can also increase your risk.
If you have one (or more) of these risk factors, there is plenty you can do to reduce your risk of developing ASCVD.
What to Do. Dietary intake is a powerful weapon in your fight against ASCVD. Include plenty of minimally processed foods like fruits, vegetables, beans, nuts, seeds, and whole grains, as well as fish and yogurt.; consume poultry, cheese, and other dairy in moderation and red meat only occasionally; and avoid processed meat and processed foods high in refined grains, starches, sugars, and salt. “Think in terms of a healthy overall dietary pattern—not, ‘this food I have to eat’ and ‘this food I have to give up forever.’” says Alice H. Lichtenstein, DSc, senior scientist and director of the Cardiovascular Nutrition Team at the HNRCA and executive editor of Tufts Health & Nutrition Letter. “It’s a balance between more of the healthier choices and fewer of the less healthy choices.”
In addition to a healthy dietary pattern, regular physical activity also supports cardiovascular health. Every movement counts (see Small Amounts of Physical Activity Can Have Big Benefits on page 4 for more information).
Shedding excess body fat reduces the burden on your blood vessels and your heart, helping lower blood pressure. It also helps lower inflammation and improve blood sugar control.
When lifestyle modifications are not enough to control LDL cholesterol levels, blood pressure, or glucose levels, medications are necessary to reduce ASCVD risk.
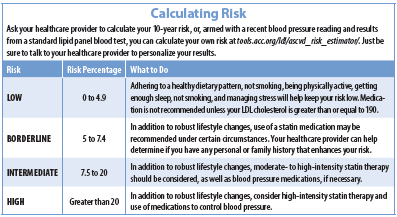
Calculating Risk. The American Heart Association and American College of Cardiology created a calculator that helps predict your 10-year ASCVD risk. The results help your healthcare provider determine the need for and intensity of treatment for high LDL cholesterol and high blood pressure. The algorithm considers your sex, age, race, total and HDL cholesterol levels, systolic blood pressure, and personal history of smoking, diabetes, and treatment for hypertension. “People who score above 7.5 percent are, on average, more likely to benefit from medication to reduce their risk,” says cardiologist Donald Lloyd-Jones, MD, president of the American Heart Association and chair of the Department of Preventive Medicine at Northwestern University, who helped develop the algorithm.
It’s important to have a knowledgeable healthcare provider conduct the assessment, or at least interpret your results. “While the score provides a 10-year estimate of risk, it needs to be put into context,” says Lloyd-Jones. “Your personal and family history may contain risk factors not included in the risk calculation, such as a personal history of rheumatoid arthritis, gestational diabetes, or chronic kidney disease, or a family history of early-onset heart attack or stroke. A knowledgeable professional can make those determinations.”
In sum, ASCVD is a common and life-threatening condition. A healthy lifestyle helps to prevent and treat this condition—and it’s never too late to start. Talk to your healthcare provider—with or without the help of the ASCVD Risk Calculator—to understand your risk and to determine the most important lifestyle changes for you, as well as whether or not medications are needed.