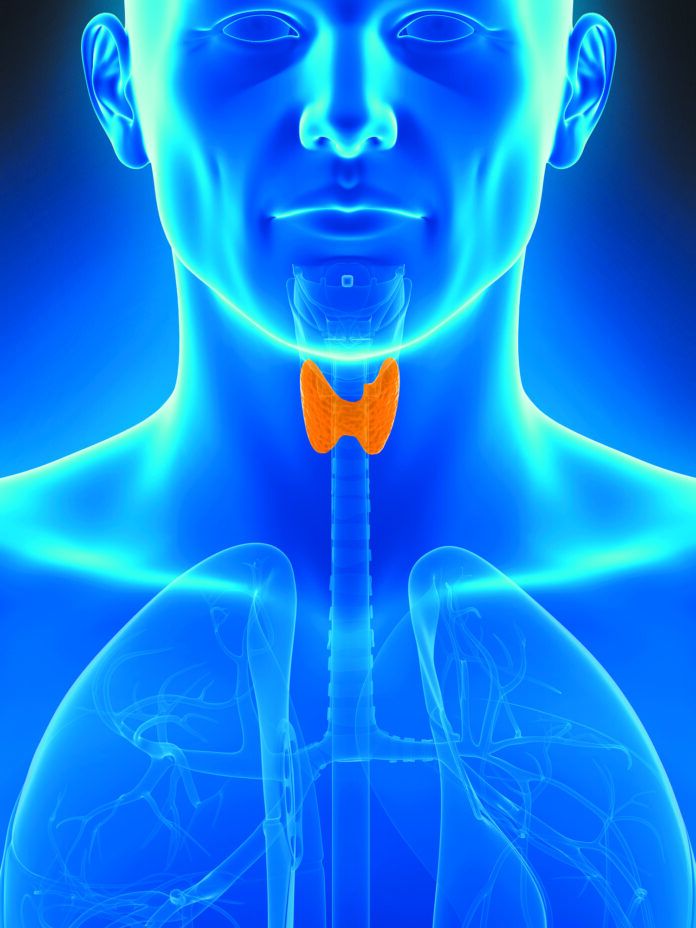
The thyroid gland curls around your windpipe just below your Adam’s apple. This butterfly-shaped gland makes and stores hormones that help control heart rate, blood pressure, body temperature, bone building, and metabolism. Modern medications and treatments make most thyroid problems treatable, but some confusion exists as to where diet fits into thyroid disease prevention and treatment.
What Can Go Wrong. If your gland is cranking out too much thyroid hormone, you may experience symptoms like unexplained weight loss, high blood pressure, rapid heart rate, palpitations, bulging eyes, sleep disturbances, irritability, anxiety, restlessness, hair loss, excessive sweating, and heat aversion. The most common cause of this hyperthyroidism is an autoimmune condition called Graves’ disease, although thyroid nodules can also cause excess hormone production.
Hypothyroidism is much more common, particularly in women over 60. An autoimmune condition called Hashimoto’s disease, resulting in an underactive thyroid, is the most common cause. Hypothyroidism can also be caused by a malfunctioning pituitary gland, inflammation of the thyroid gland (thyroiditis), and side effects of some medications. Other symptoms include weight gain, swollen neck due to an enlarged thyroid gland (goiter), low heart rate, depression, tiredness, feeling cold, dry skin, and brittle nails.
Don’t overdo it! Avoid unprescribed iodine and selenium supplements, and don’t eat large amounts of seaweed or Brazil nuts regularly.
Choose iodized salt. The addition of iodine to table salt made hypothyroidism rare.
Enjoy soy. The isoflavones in soy have not been found to increase risk for thyroid problems.
Eat plants. A healthy diet high in minimally processed plant-based foods may be protective against autoimmune conditions like common thyroid diseases.
Diet and Your Thyroid. The internet is full of lists of foods to eat or avoid (and supplements to take) if you have (or want to avoid) thyroid problems. Let’s look at the science behind some popular pitches:
Iodine: The body can’t make thyroid hormone without this essential trace element. Iodine deficiency causes hypothyroidism. In the 1920s, the U.S. government recommended the addition of iodine to table salt, virtually eliminating iodine deficiency in the country. Since most adults in the U.S. already exceed the daily recommended 150 micrograms (mcg) of iodine (consuming about 216 mcg a day, on average), there is no need to seek out high-iodine foods or take iodine supplements. Iodine intake above 1,100 mcg a day over a long period of time is unsafe and, in some cases, may itself lead to hypothyroidism. (Some seaweeds have this much in one serving, but to get over 1,000 mcg of iodine otherwise would generally require taking supplements.) Iodized salt is recommended. If you use sea salt, which does not contain iodine, be sure to occasionally include some iodized salt in your cooking.
Selenium: Deficiency of this essential mineral can cause thyroid dysfunction, but selenium deficiency is very rare in the U.S. A recent trial found selenium supplementation had no significant benefit for participants at risk for hypothyroidism. Most people in the U.S. already exceed the daily recommended intake of selenium (55 mcg for adults). Intake of over 400 mcg a day is considered unsafe. Frequently consuming large numbers of Brazil nuts could lead to selenium toxicity, but it is otherwise difficult to overdo this nutrient if you’re not taking supplements.
Isoflavones: Much has been written about the isoflavones in soy inhibiting the production of thyroid hormones, but a 2021 review of research found no evidence that this is the case. There is no reason to avoid soy products if you have hypothyroidism, unless you are instructed to do so by your healthcare provider.
Gluten: Celiac disease is more common in people with autoimmune thyroid disease than in the general population. However, research does not support the idea that avoiding gluten will help prevent or treat thyroid disorders.
What to Do. In a recent study, participants with Hashimoto’s thyroiditis reported a higher intake of animal foods than healthy controls, while participants without thyroid disorders were more likely to report higher intake of plant foods. A healthy plant-based diet, therefore, is a good choice for thyroid (and overall) health.
If you are taking thyroid hormones, take them at least two hours before or after eating. Thyroid hormones should not be taken at the same time as calcium or iron supplements, antacids, or some medications (your healthcare provider or pharmacist can advise you).
If you have symptoms of thyroid disorder or a family history of thyroid disease, check with your healthcare provider to see if they recommend testing your blood for levels of thyroid stimulating hormone (TSH). Other than avoiding excessive regular consumption of seaweed and Brazil nuts, no dietary changes are necessary to avoid or treat thyroid problems (unless specified by your healthcare provider).