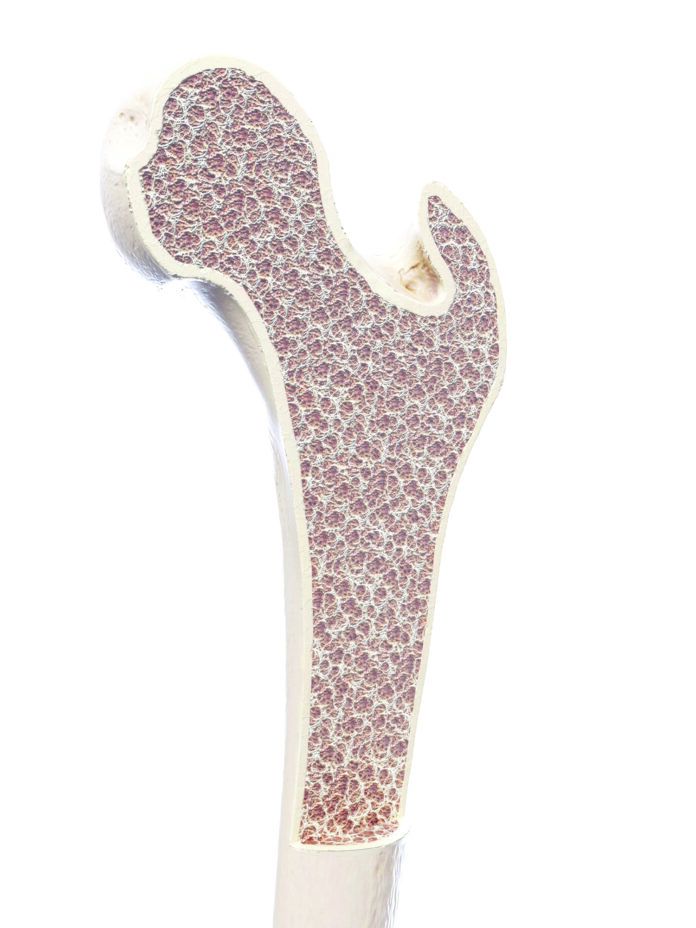
Osteoporosis is characterized by a decrease in bone density. It affects 12.6 percent of community-dwelling adults over 50 and 27.1 percent of women over 65 in the U.S. (for men over 65, the prevalence is 5.7 percent). People with osteoporosis are more likely to suffer bone fractures, which can lead to loss of independence, reduced ability to perform activities of daily living, and even death.
After reviewing all available evidence, the U.S. Preventive Services Task Force (USPSTF) has concluded that routinely screening women 65 years and older for osteoporosis could help prevent osteoporotic fractures by identifying at-risk individuals. Postmenopausal women younger than 65 years who are at increased risk for an osteoporotic fracture could also benefit from routine screening. (Risk factors include low body weight, parental history of hip fracture, cigarette smoking, excess alcohol intake, diabetes treated with insulin, or corticosteroid use.) There is not currently enough evidence to determine if screening would be beneficial for men.
The USPSTF is an independent panel of experts that makes recommendations about the effectiveness of preventive care services. This recommendation was made based on the results of a systematic review evaluating the benefits and harms of screening for osteoporosis to prevent fractures in adults 40 years or older who do not have a known history of the disorder.
If you are a woman aged 65 or older, talk to your healthcare provider about getting screened for osteoporosis. The most common screening test is a DEXA scan (dual-energy x-ray absorptiometry). This test uses low doses of radiation to measure bone density at a central site, like the hip, neck, or lumbar spine. Postmenopausal women under 65 who have other osteoporosis risk factors should also talk to their healthcare provider about the appropriateness of screening.